PROJECT
From the Covid-19 pandemic, European countries learnt the importance of flexibility in funding and organization of health systems, but there are still several challenges for healthcare systems that require efficient and flexible financing mechanisms to be successfully addressed:

The Project
The FLASH project intends to be a game-changer in the European integrated healthcare system.
By focusing on budget allocation and financing of health services within a specific budget with a multidisciplinary approach, the project conducts an extensive investigation of healthcare financing mechanisms across Europe.
It tries to pinpoint and investigate the most significant factors that underline the link between the major problems facing healthcare systems and their funding.
It also intends to provide evidence on the ability of existing financing mechanisms and contracts to address such challenges and study new solutions to achieve more effective, efficient and equitable healthcare systems.

Objectives

Expected Results

Work Plan
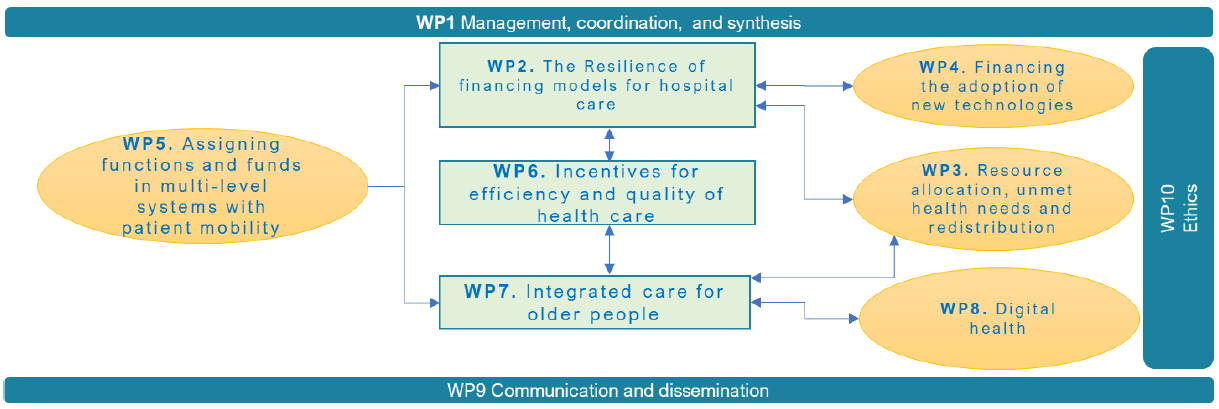
The FLASH project consists of 10 Work Packages (WPs):
The connections between WPs are shown in the Workflow diagram below.